Calciphylaxis is a clinical problem with increasing incidence in elderly patients, patients with vascular disease and haemodialysis patients. The treatment of choice should be multidisciplinary.1,2 The main agent is intravenous sodium thiosulfate (ST); however, it may be poorly tolerated. Here we discuss the possibility of using ST adjuvant treatment.
73-Year-old woman on chronic haemodialysis for end-stage renal failure (diabetic and chronic interstitial nephropathy). Hypertension, hypertensive heart disease, type 2 diabetes mellitus, diabetic neuropathy, chronic revascularised ischaemic heart disease, severe atheromatous of the aorta and visceral branches with mesenteric angina and microscopic colitis, transient ischaemic attack, peripheral vascular disease and severe hyperparathyroidism. Treated with carvedilol, clopidogrel, simvastatin, ezetimibe, omega 3 fatty acids, paricalcitol, cinacalcet, omeprazole, insulin, repaglinide, lanthanum carbonate, transdermal nitroglycerin, oral budesonide, calcifediol, erythropoietin and intravenous iron and carnitine.
Dialysed through a outer humeral gore-tex prosthesis with online haemodiafiltration, for 3h, 4 times a week, with high-permeability polysulfone, anticoagulation with enoxaparin, and calcium bath 1.5mEq/L.
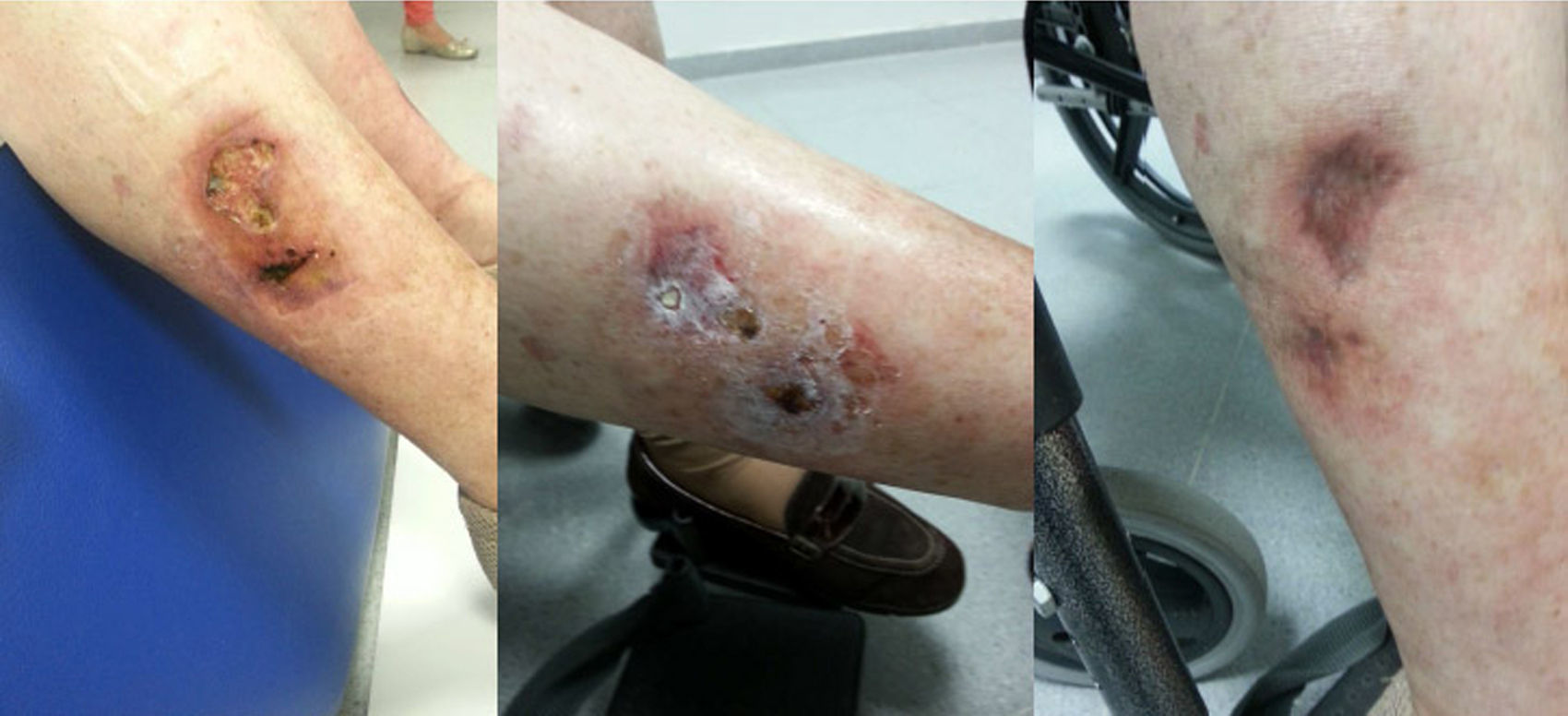
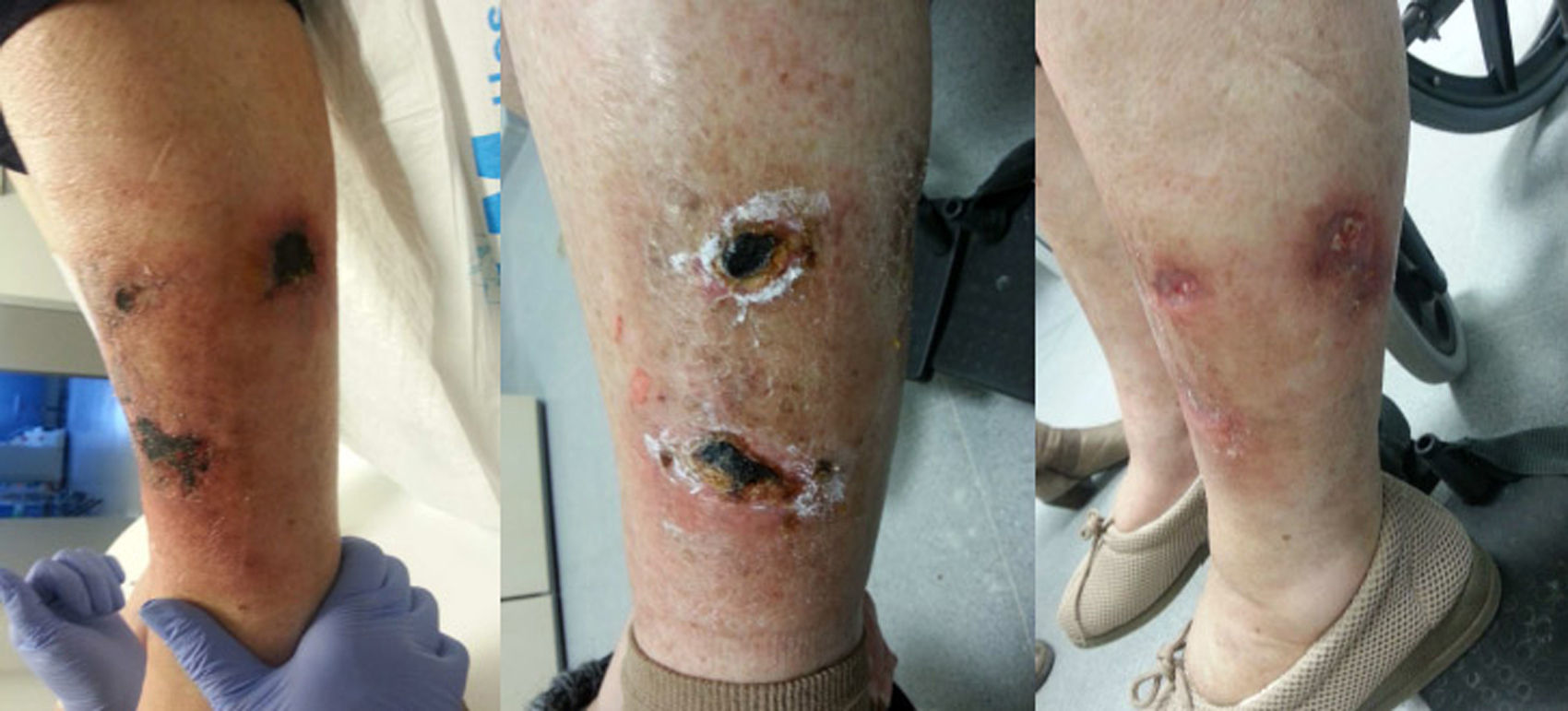
At 18 months she had a painful macular lesion in the distal third of the right leg, which became ulcerated. Diagnostic biopsy revealed atherosclerotic vascular disease, treated conservatively and stabilised. Five months later she received a kidney transplant hat was technically difficult due to severe calcification. Immunosuppression was induced with basiliximab, steroids, tacrolimus, and mycophenolic acid, and kidney function stabilised at Cr 1.2mg/dL (MDRD-IDMS 55ml/min). In the following weeks the ulcer worsened and 3 more lesions appeared on the legs, which were very painful, necrotic that rapidly worsened. A second biopsy showed calciphylaxis, and so oral bisphosphonate and intravenous ST at doses of 7.5g/session/2 sessions per week for 4h were started. She developed metabolic acidosis, severe gastrointestinal intolerance, low blood pressure and general deterioration. The dose of ST was reduced and bed-rest was indicated after each session. No improvement with bicarbonate or ondansetron supplements; so after 50 days of treatment, during which she received 135g for 18 sessions, the ST iv was suspended and topical ST started (magistral formula: 25%, based on Beeler). Occlusive dressings every 12h, alternating with debriding ointment (Dertrase®) for 90 days. Now the patient is doing very well, with less pain and with the lesions resolving without significant complications (Figs. 1 and 2).
Calciphylaxis, or uraemic gangrene or calcific uraemic arteriolopathy,3 is a necrosis of fat caused by hypoperfusion that primarily affects the proximal areas of the legs. The diagnosis was made by biopsy, in which we found necrosis of the epidermis, dermis and hypodermis, intimate fibrodysplasia, micro-thrombosis and calcium deposition in the small arterioles and panniculitis.2 She presented with livedo reticularis, subcutaneous nodules and plaques that lead to necrosis and cause deep necrotic ulcers.
The following are risk factors for their development1,2: kidney failure (1–4% incidence in haemodialysis and 1.3–4.5% a year in advanced chronic kidney failure),4 low blood pressure, abnormal calcium and phosphorus product, metabolic syndrome, female gender, Caucasian and treatment with vitamin D, calcium, warfarin or acenocumarol. It can be associated with cirrhosis, Crohn's disease, hyper- or hypoparathyroidism, kidney transplantation, autoimmune diseases, thrombophilia, intravenous iron overload, Hodgkin lymphoma and gastric bypass, among other conditions.1,2
Treatment should be multidisciplinary, treating the infection early, ensuring adequate nutrition, suspending vitamin D and calcium, adding bisphosphonates and, for haemodialysis patients, using a low calcium bath and dialysing daily. Other measures include iloprost, cinacalcet, statins, non-calcium phosphorus chelating agents, common green bottle fly (Lucilia sericata) larvae,1 diltiazem, colchicine and ceftriaxone2 and ST, preferably intravenously.
ST has been used intravenously since 2004 due to its vasodilator and antioxidant effects. It is dialysable (molecular weight: 248Da) and has a half life of 15min with preserved glomerular filtration rate (GFR). Renal clearance is 95% and bile clearance 2%5; it generates acid metabolites (thiosulfuric acid) that last for hours. A dose of 25g 3 times a week in haemodialysis and preserved GF, in a slow infusion, is recommended. For a GF less than 60ml/min/1.73m2 the initial dose is 12.5g/2 times a week.
It may cause acidosis, gastrointestinal intolerance, headache, phlebitis, hypocalcaemia, hypoglycaemia, QT prolongation and abnormal bone mineralisation.
There are reported cases of oral administration,6 intralesional injection7 and occlusive dressing with emulsion-based zinc oxide, in other ailments,8,9 for 11–24 weeks, with cost saving and no complications.
In our case, the IV route was poorly tolerated, which meant a small cumulative dose (there are cases of 1268±1555g cumulative dose),10 and therefore we had to explore other possibilities to prevent previous undesirable effects.
We believe that administration of topical ST is an economical, safe treatment that should not be dismissed as an alternative in selected cases.
Conflicts of interestThe authors declare that they have no conflicts of interest.
Please cite this article as: Martín Navarro JA, Pedraza Cezón LA, de Pablos Martín MP, González Monte E, Polanco Fernández N, Gutiérrez Sánchez MJ, et al. Tratamiento con tiosulfato de sodio tópico en calcifilaxia de paciente con trasplante renal activo. Nefrologia. 2016;36:579–581.