Introducción: Cuando un paciente en hemodiálisis sufre la trombosis de su fístula arteriovenosa (FAV), necesita algún procedimiento urgente para su próxima sesión de diálisis. Existen dos opciones terapéuticas: la colocación de un catéter venoso central (CVC) o la reparación de su FAV. El objetivo de este trabajo es valorar la posibilidad de reparación urgente de las FAV trombosadas dentro de la actividad de urgencias de un servicio de cirugía general y determinar la posible repercusión económica de la implantación de este protocolo de trabajo en un área sanitaria. Método: Se realizó la recogida prospectiva de todas las intervenciones quirúrgicas urgentes realizadas para la reparación de las FAV trombosadas en el período 2000-2011 en nuestro centro. Se analizaron los resultados clínicos mediante dos variables: tasa de trombosis (episodios/paciente/año) y porcentaje de rescate. Se consideró un rescate eficaz si tras la intervención el paciente se pudo dializar con su FAV evitando la colocación de un CVC. Se definió e implantó el proceso clínico «FAV trombosada» y se estudió su coste económico mediante un análisis detallado realizado por el departamento económico financiero de nuestro centro. También se realizó este análisis para el proceso clínico alternativo (nueva FAV) utilizando los datos publicados por el Ministerio de Sanidad (peso del Grupo Relacionado con el Diagnóstico: accesos vasculares para hemodiálisis, unidad de complejidad hospitalaria, precio público de procesos ambulatorios y porcentaje de cirugía ambulatoria). Finalmente se realizó una estimación de la repercusión económica de la implantación de este proceso comparando los costes de ambos procedimientos. Resultados: Durante el período de estudio se produjeron 268 episodios de trombosis, lo que supone una tasa de 0,10 episodios/paciente/año (0,05 en FAV autólogas y 0,43 en injertos). Se atendieron de forma urgente por el servicio de cirugía 203 (75 %), consiguiendo rescatar 168 FAV (82 %). El coste de una reparación urgente de una FAV se estimó en 999 €. El precio promedio de una FAV programada más el precio de la colocación y mantenimiento de un CVC se estimó en 6397 €. El ahorro producido por la reparación urgente de las FAV en nuestra área de salud es de 107 940 €/año. La extrapolación al conjunto del país para una población de 23 000 pacientes en hemodiálisis sería de 9 930 480 €/año. Conclusiones: Es posible realizar el rescate quirúrgico urgente de la mayoría de las FAV para hemodiálisis. La implantación de un protocolo multidisciplinar evita la colocación de catéteres en estos pacientes, disminuyendo el gasto asociado a ellos.
Introduction: When a patient undergoing haemodialysis suffers from arteriovenous fistula (AVF) thrombosis, (s)he needs an urgent procedure before the next dialysis session. Two different treatment options are available: placing a central venous catheter (CVC) or repairing the AVF. The objective of this study is to assess the possibility of urgent repair of thrombosed AVFs within the emergency care activity of a general surgery department and to determine the possible economic repercussions of implementing this working protocol in an area of healthcare. Method: We completed the prospective collection of all the urgent surgical interventions made to repair thrombosed AVFs for the period 2000-2011 at our centre. The clinical results were analysed using two variables: rate of thrombosis (episodes/patient/year) and percentage of recovery. Recovery was deemed effective if after the surgery the patient was able to undergo dialysis of his/her AVF without the need to place a CVC. The “thrombosed AVF” clinical process was defined and implemented, and its economic cost was analysed via a detailed analysis conducted by our centre’s Financial Department. This analysis was also conducted for the alternative clinical process (new AVF), using the data published by the Ministry of Health (weight of the Diagnosis-Related Group: vascular accesses for haemodialysis, hospital complexity unit, public cost of outpatient procedures and percentage of economic repercussions of the implementation of this process, comparing the costs of both procedures). Results: During the study period 268 episodes of thrombosis occurred, a rate of 0.1 episodes/patient/year (0.05 on autologous AVFs and 0.43 on grafts). 203 (75%) were treated urgently by the surgery department, of which 168 AVFs (82%) were recovered. The cost of urgently repairing an AVF was estimated at €999. The average cost of a scheduled AVF intervention, plus the cost of placing and maintaining a CVC, was estimated at €6,397. The saving made by urgent repair of AVFs in our area of healthcare is €107,940/year. Extrapolating this to the entire country for a population of 23,000 patients on haemodialysis, the total would be €9,930,480/year. Conclusions: It is possible to perform urgent surgical recovery on the majority of AVFs for haemodialysis. Implementing multidisciplinary protocol avoids fitting these patients with catheters, reducing the cost this entails.
INTRODUCTION
Despite the improvement in monitoring protocols, thrombosis continues to be the most common complication of arteriovenous fistulae (AVF), varying between 0.1 and 0.2 episodes per patient and year in our setting1,2. The absence of radiological and surgical support and protocols in most haemodialysis units results in a considerable number of hospitalisations, central venous catheter (CVC) related morbidity and consequentially, increased healthcare costs. Bearing in mind the importance of AVF to haemodialysis patients, central venous catheter-associated morbidity and anatomical limitations of multiple accesses, our clinical guidelines consider AVF thrombosis to be a medical emergency3: Recommendation 5.2.1.- “The restoration of patency must be attempted in any thrombosed vascular access in which this is feasible, provided that it is not contraindicated. Vascular access thrombosis must be considered as a medical emergency and the recovery procedure must be carried out immediately. Evidence B”. This is probably one of the most important and forgotten recommendations. In summary, whenever a patient comes to their haemodialysis unit with a thrombosed AVF, a clinical process begins that has two basic routes:
The objective of this study was twofold: to assess the possibility of urgently repairing thrombosed AVF within the emergency activity of a general surgery department and to estimate the economic costs associated with these two clinical processes. Our endeavour was not to analyse the clinical consequences of catheter use; the proof of this does not require further justification4.
METHODS
Setting
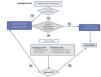
Area 8 of the Community of Madrid with a population of 550,000. Since our hospital was opened, emergency care for these patients has been considered part of the range of services offered by the surgery department and a protocol has been established5. Various surgeons have taken an interest in this issue and work to treat this pathology. There are no specific shifts for treating these patients. Treatment of AVF complications is added to the regular activity of the general surgery service. The team on duty in our hospital comprises two general surgeons. We collected all cases of AVF thrombosis prospectively in a single database for the whole area. We defined and implemented thrombosed AVF and new AVF clinical processes6 (Figures 1 and 2). The unit’s mean vascular access distribution over these years was: 65% autologous AVF, 15% grafts and 20% CVC.
Analysis of clinical results
All episodes of thrombosis were included by the nephrology department and all emergency surgical recovery procedures were included by the surgery department, in order to calculate the percentages of each technique, in a specific form for haemodialysis vascular access since the hospital opened. The recovery was considered to be successful if the AVF could be used in at least the next three dialysis sessions, with catheterisation being avoided. We analysed the thrombosis rate (episodes/patient/year) to estimate the cost in our area.
Cost analysis
Cost of emergency surgery: we were able to analyse the costs of emergency AVF repair thanks to the detailed study by the hospital’s financial department. We analysed the cost of the consumables and expanded polytetrafluoroethylene grafts (PTFE 6mm x 10cm GORE-TEX® Stretch Vascular Graft) used in the worst case scenario (that one is used in each procedure). The staff cost in our case was considered to be zero, since there are no specific shifts or extra remuneration for performing these procedures or altering productivity of the remaining emergency activity. Cost of scheduled surgery: we analysed the costs of the new vascular access process when emergency repair is not carried out (including catheter insertion and maintenance, surgery and anaesthesia consultations and the scheduled surgery procedure). We included correction factors to achieve an average cost based on the replacement rate (outpatient percentage) of each procedure. The sources for this analysis are data published by the Ministry of Health and the Health Department of the Autonomous Community of Madrid (public costs of scheduled outpatient procedures, replacement rates, hospital complexity unit cost [HCU = €2116.28] and diagnosis-related group [DRG] 315 weight)7. Creation of an AVF is included in the DRG (diagnosis-related group) code n.º 315 “Other kidney and urinary tract surgical procedures”, with an assigned weight of 2.8909. It is a surgical DRG that groups patients admitted due to kidney or urinary tract disease, who received an operation such as: creation of an AVF for dialysis or a peritoneal-cutaneous fistula, percutaneous angioplasty in peripheral arteries, a bone biopsy, a laparotomy or a laparoscopy. Furthermore, we added to the costs of the process (when the AVF is not repaired), the cost of surgery and anaesthesia consultations, as well as that of inserting and maintaining a tunnelled catheter during the waiting period8. Lastly, we estimated the annual savings made in emergency activity. To do this, we compared the costs of the processes described to find out the savings made per process and we multiplied this figure by the estimated number of processes according to our thrombosis rate. This figure was extrapolated to the haemodialysis population of the whole country9.
RESULTS
Between the years 2000 and 2011, there were 268 episodes of AVF thrombosis in our hospital, 196 in autologous AVF and 72 in grafts, resulting in a rate of 0.10 episodes/patient/year (0.05 in autologous AVF and 0.43 in grafts). The surgery department performed emergency operations in 203 episodes (75% of the total) and 168 AVF (82%) were recovered, without a catheter being inserted. We do not know what percentage of the 25% of thromboses were not operated on due to an absence of qualified staff and what percentage was the result of considering the AVF to be non-recoverable or a poor patient condition.
Costs of the emergency process
Cost of the emergency outpatient surgery process:
Consumables: €64. Prosthesis: €367. Total cost of emergency surgery: €431. In our experience, 90% of these procedures are performed without patient admission. We added a correction factor of 10% for procedures with patient admission.
Cost of emergency outpatient surgery (€431) x 0.9 = (€387.9) +
Cost of emergency inpatient surgery (HCU x DRG weight) = €6117.95 x 0.1 (€611.795)
Average cost of emergency surgery €387.9+611.795 = €999.695.
Cost of the scheduled major outpatient surgery (MOS) process: Public cost of outpatient procedures. The public cost of outpatient (MOS) DRG 315 is €1438.
Cost of the inpatient process: This was obtained by multiplying the cost of the hospital complexity unit by the DRG 315 weight.
2012 HCU price (€2116.28) X weight (2.8909)= €6117.95.
Average cost of the scheduled surgery procedure: we took into account the replacement rate published in the outpatient surgery manual of the Ministry of Health.
Replacement rate (outpatient percentage) DRG 315= 46%.
Cost of scheduled outpatient surgery (€1438) x 0.46 = €661.48 +
Cost of inpatient surgery (6117.95€) x 0.54= €3303.693.
Average cost = €3965.163.
Cost of consultations: €90
Cost of insertion and maintenance of catheter: €563/month (8)
Final cost of the scheduled procedure
Average cost of surgery (3965.163). + Consultation cost: €90x2 + Cost of insertion and maintenance of the catheter: €563 x 4 months = €6397
Estimation of annual savings
The added cost for each patient without “recovery” was calculated by subtracting the cost of the emergency procedure from the cost of the process for a new AVF: 6397 - 1000 = €5397. Savings in our health area were calculated by multiplying the savings per procedure by the number of thrombosis episodes recovered: health area savings 500,000 (250 patients): 25 episodes/year (x 0.8) AVF recovered: 20/year x 5397 = €107,940/year. When we extrapolate this figure to the whole country for a population of 23,000 haemodialysis patients, the cost would be €9,930,480/year.
DISCUSSION
Although there is no doubt that the best treatment of AVF thrombosis is prevention through applying monitoring methods10, whenever a patient has a thrombosed AVF, the nephrologist is faced with the dilemma of trying to repair it or inserting a CVC for the next session. Clearly, the best option from the clinical point of view is to repair the AVF and this is what the clinical guidelines of the Spanish Society of Nephrology recommend3. However, this is not always possible, and in fact, in most units of the Autonomous Community of Madrid, there is no radiological or surgical support with protocol for addressing this situation2. It is hard to know why this situation has persisted and even deteriorated, but in general, nephrologists have become resigned to it and surgical departments are not motivated to change2. So much so that even the scientific debate on the treatment of AVF thrombosis is focused on the method employed (radiological or surgical)11 and it neglects the basic aspect of considering it an emergency. In our experience, the results are consistent with the recommendations of national and international clinical guidelines. Our economic situation is different from that of the United States, where most maintenance procedures are radiological12, but a surgical approach is more profitable from a cost/benefit point of view because of the low cost of the material used, low rates for medical staff and fewer procedures to maintain a similar secondary patency13,14.
Our study demonstrates that repair or recovery is possible in most AVF, even in complex cases requiring operations that last more than 2 hours (thrombectomy and PTFE insertion in the proximal axillary vein, partial PTFE replacements) and we believe the scientific literature available on the damage caused by CVC in haemodialysis patients. Aside from the decreased morbidity in our patients, which is not the subject of this study, it has been shown that this process results in a clear decrease in costs associated with vascular access for haemodialysis. Our zero staff cost model is not exportable because it depends on the voluntary effort of a small group of surgeons, but the figures show that in reference centres for several units, expenditure on additional staff with a specific shift would be more than justified for addressing this issue. There are data used to estimate expenditure in this study that may be criticised due to bias:
- Thrombosis rate: to calculate savings in our area, we used our data and then extrapolated them to the general population. These were quite similar to others published1,2 and in any case, it seems that the figure is an underestimation, since in most registries, the person who communicates the results is usually the person who best monitors the situation and it is therefore to be expected that the rate in the country is higher than 0.1.
- Waiting time: also taken from our data, this is similar to the data reported by Rodríguez and in any case, it seems that in the current economic climate, it may be higher.
- Staff cost. This would be an additional cost if reference centres with a specific shift were created. This is not the case for us and it is reflected as such in the cost analysis. It could be argued that our shifts are paid and that the cost is therefore not zero. In response to this, we would have to say that this activity is added and does not detract from our regular emergency activity. Neither is more pay received for doing what is not done in other hospitals.
- Outpatient percentage. Our costs are lower, amongst other reasons because of the high outpatient percentage compared with that published by the Ministry of Health in its outpatient surgery manual. We used our data with a current outpatient emergency surgery rate of almost 90%, which is an improvement on previously published figures15.
Based on the study results, independently of attempting to achieve a decrease in the thrombosis rate, we propose some areas for improvement in AVF maintenance management:
CONCLUSIONS
Conflicts of interest
The authors declare that they have no conflicts of interest related to the contents of this article.
Figure 1. Thrombosed arteriovenous fistula process.
Figure 2. New arteriovenous fistula process.