The current outbreak of SARS-CoV-2 represents a special risk for renal patients due to their comorbidities and advanced age. The usual performance of hemodialysis treatment s in collective rooms increases the risk. The specific information at this time in this regard is very limited. This manuscript includes a proposal for action to prevent infection in the Nephrology Services, and in particular in hemodialysis units, with the objective of early identification of patients who meet the definition of a suspected case of infection by SARS-CoV-2 and propose circuits and mechanisms to carry out hemodialysis treatments. They are recommendations in continuous review and can be modified if the epidemiological situation, the diagnostic and therapeutic options so require.
La epidemia de SARS-CoV-2 representa un riesgo especial para los pacientes renales por su condición de personas con comorbilidades y edad avanzada, y por la realización del tratamiento de hemodiálisis en salas colectivas. La información específica en el momento actual al respecto es muy limitada. El presente manuscrito recoge una propuesta de actuación para prevenir la infección en los Servicios de Nefrología, y en particular en las Unidades de Hemodiálisis, con el objetivo de identificar precozmente aquellos pacientes que cumplan con la definición de caso sospechoso de infección por el SARS-CoV-2 y proponer circuitos y mecanismos para administrarles el tratamiento con hemodiálisis. Son recomendaciones en continua revisión y podrán ser modificadas si la situación epidemiológica y las opciones diagnóstico-terapéuticas así lo requieren.
On January 31st 2020, the World Health Organization declared the outbreak of SARS-CoV-2 in China, a public health emergency of international dimension.1 According to the information provided by the China Center for Disease Control and in more recent publications, the majority of cases reported came from the Hubei province and in 80% the disease was mild. The proportion of deaths among confirmed cases has fluctuated between 2 and 3%, being higher in Hubei than in the rest of the country that reported a 0.4%. Most cases detected in China are older than 30 years, and among severe and deceased cases there is a high proportion of patients with comorbidities and advanced age.2,3 To date the hemodialysis cases reported are from a Hubei hemodialysis center, in which 37 out of 230 dialysis patients, tested positive for COVID-19 in addition 4 of the 33 health personnel were also positive. Six patients with COVID-19 die (16.8%) mainly from cardiovascular causes, with less probability of developing pneumonia than the general population.4
Up to now, the source of infection is unknown and there is uncertainty about the severity of the disease and the capacity of virus transmission. As other known coronaviruses, SARS-CoV-2 is believed to be transmitted primarily by respiratory droplets larger than 5 microns and by direct contact with the secretions of infected individuals. Other possible transmission routes are being evaluated. The incubation period of the disease in the first cases has been estimated at 2–14 days.5
The Ministry of Health of the Government of Spain publishes periodically a technical report describing actions to adopt; no special indication for dialysis units have been included at this time.6 American Society of Nephrology has issued a note with frequently asked questions and some guidelines7 very similar to the Center for Diseases control in Europe and USA8,9 and there are recommendations made by the Nephrology Societies of Taiwan and China. The present manuscript contains a proposal for action to prevent infection in Nephrology Services particularly Hemodialysis facilities. These hemodialysis centers are especially prone to transmission and these patients are a high-risk population with associated comorbidities.2,4
The proposal what we consider pertinent at the time of its drafting. With this changing epidemic development, some of the proposed approaches could be overcome in the short term by the real upcoming events. The recommendations included in this document are aligned with the general protocol for the detection and management of SAR-CoV-2 infection at the Hospital del Mar in Barcelona.10 These are under continuous review and may be modified according to the epidemiological situation and therapeutic options.
The objectives are: first, early identification in the Nephrology Service of suspected patients (including those cases considered by the Ministry of Health as cases under study, probable or close contact) or patients confirmed to be infected by SARS-CoV-2. Second, propose circuits and mechanisms for administration of hemodialysis treatment with the objective of minimizing the risk of contagion to other patients on hemodialysis and to the staff.
Early actionsIt is essential to have and adequate training of all professional in the hemodialysis unit on the prevention and identification measures of COVID-19 is essential.
It is highly advisable to have one or two of the following options: (1) a portable ambulatory hemodialysis monitor with bags to be able to dialyze anywhere in the hospital without the need of relocating the patient and maintain isolation and (2) a box for adequate hemodialysis under conditions of contact and drop isolation.
As any health professional nurses and doctors attending dialysis facilities should wash their hands with soap and water and applied alcoholic solutions systematically.
Advices to hemodialysis patients- •
Receive your seasonal flu vaccine (H. influenza) every year at the outpatient clinic.
- •
Wash your hands frequently with soap and water for at least 20s, and ideally 60s. If soap and water are not available, use an alcohol-based hand sanitizer.
- •
Avoid touching your eyes, nose, and mouth with your unwashed hands.
- •
Avoid close contact with sick people with respiratory symptoms.
- •
If you are sick stay at home and phone the dialysis center, and they will provide you with appropriate recommendations.
- •
If after informing you have been authorized to attend the dialysis center, do not use public transportation (contact individual ambulance to be transferred to the Emergency Service of the hospital). If you use your own vehicle, after arrival do not wait with other patients in the general waiting room.
- •
If you cough or sneeze, cover your mouth and nose with your sleeve or a tissue, then throw it away.
- •
Objects and surfaces that are frequently touched should be cleaned and disinfected with water and bleach or any household disinfectant.
- •
If you develop any respiratory symptoms or low degree fever, if you have had close contact (less than 2m) with a probable or confirmed case, or if you or someone close to you has recently been traveling, immediately inform the medical staff of the hemodialysis. Areas of heavy transmission change as the epidemic evolves, so regular updates are required.
- •
Wash your hands with soap and water for at least 20s before entering the ambulance and before entering the unit. If soap and water are not available, use an alcohol-based hand sanitizer.
Patients may have a wide spectrum of symptoms, from asymptomatic infection to severe clinical symptoms of fever, cough, and shortness of breath, although most cases the symptoms are limited to fever and mild cough. Symptoms may appear in only 1 day or up to 14 days after exposure, however the average incubation period is 5–6 days.5
To identify patients that could be infected with SAR-Co V -2 the following measures will be observed prior to the entry into the Dialysis Unit:
- 1)
Nursing personnel equipped with gloves and mask will interrogate all patients about:
- -
Sudden onset of any of the following symptoms: cough, fever and/or, dyspnea, of any intensity.
- -
Relevant information about the 14-day period prior to the onset of symptoms relative to epidemiological measures:
- ∘
Travel history to areas with evidence of community transmission, as previously discussed.
- ∘
History of close contact (less than 2m) with a probable or confirmed case.
- ∘
- -
- 2)
Infection will be suspected in any person requiring hospitalization for severe acute respiratory infection (pneumonia, distress acute respiratory failure syndrome multiorgan, septic shock, ICU admission or death) in whom other possible infectious etiologies have been ruled out.
- 3)
In the hemodialysis unit:
- •
Place a sign at the entrance (in different languages, according to the needs of each unit) directed to individuals with clinical and epidemiological criteria of possible SARS-CoV-2 infection (example in Fig. 1), so that they can alert the staff so the necessary precautions are implemented.
- •
Place containers with hydroalcohol solution in the patients waiting room and instruct them how to use it.
- •
If patients have fever or respiratory symptoms, they must inform by phone the dialysis staff even before entering the public transport. The staff of the unit will be prepared for the patient arrival or classify them in a more appropriate environment (route of entrance to be designed according to hospital protocol).
- •
In these cases do not use the collective transport regularly utilized to move to the Dialysis Center; rather use individual transportation which must have separation from the driver. There will be a transport individual with the means of protection that can be offered, the minimum required is a surgical mask and gloves for the patient and companion; and a surgical mask for medical transport personnel. After completion of the transport the vehicle will be disinfected and proceed with management of waste products.
- •
All patients will enter the dialysis facilities through the locker room, where hands will be washed.
- •
If patients have symptoms (cough, fever or dyspnea), nurses will provide a surgical mask and will interrogate the patient about possible epidemiological risk (see point 1).
- •
If there is not a case identified with a suspected infection, the masks can be removed during hemodialysis to those patients who wish to do so.
- •
Staff and patients have to be informed about respiratory hygiene and the necessary material has to be provided: hand hygiene (alcohol solution has to be accessible), cover your nose and mouth while coughing or sneezing using disposable tissues, with accessible containers for these wastes.
- •
It is advisable that a nurse attends always the same patients for connection, disconnection, care during the hemodialysis session, administration of medication and so on. Patients attended by each professional in each shift should be registered; this will facilitate traceability in the event that a patient becomes infected.
- •
- 4)
In peripheral hemodialysis facilities dependent on hospital centers:
- •
It is recommended to follow the recommendations described in this procedure for patients form hospital hemodialysis units (section 3)
- •
In case of doubts and questions, contact those responsible of the hospital hemodialysis center.
- •
In the hospital hemodialysis unit:
- •
Should any suspected case be identified upon arrival to the unit, this patient will be separated from the other patients, it will be given gloves and a surgical mask and will be conducted immediately to the room or box that had been previously prepared for contact and drops isolation.
- •
If a suspected case is identified inside the unit, once dialysis has been started, the urgent need of dialysis will be assessed and in case of no urgency the patients should be disconnected and separated from to other patients. The patient will be given gloves and a surgical mask and will be immediately taken to the previously conditioned isolation room or box. Dialysis will be continued at another time.
- •
Personnel accompanying the patient to the isolation room will also wear gloves and a surgical mask, keeping a distance of 2m from the patient. Try to ensure that the patient does not touch objects (handles, doors, furniture in general, etc.) or people.
- •
As soon as possible, a respiratory smear will be performed to detect the virus by PCR, following the protocol established in each hospital for the detection, diagnosis and management of suspected cases.
In peripheral hemodialysis facilities dependent on hospital centers:
- •
Identify and select a single room in the facility that can be used to isolate a patient with suspected of SARS-CoV-2 infection (contact and drops isolation). It will be used for further evaluation of the patient while waiting to be transferred. If an isolation room is not available, the patient must be kept with a surgical mask and gloves, and separated 2m from the rest of the patients.
- •
Always notify the medical and nursing staff of the hemodialysis unit of the reference hospital before referring a patient who meets the criteria for suspected infection with SARS-CoV-2.
- •
Patients who have shared medical transport, have been less than 2m in the waiting room, or have been dialyzed in adjacent positions or beds (<2m or 2 seats) to patient with proven infection, will be considered close contacts and epidemiological surveillance agency must proceed for the screening for SARS-CoV-2 infection.
- •
Since the incubation period is of 14 days should these patients should be treated as potentially infectious and during the period of “quarantine” he should be alert about symptom and be isolated at home. Will be transported by ambulance individually with surgical gloves and mask. The patient will be dialyzed separated from the rest of the patients, preferably in the last shift of the day (if necessary in night shifts), taking extreme measures of disinfection and subsequent cleaning of the hemodialysis facility.
- •
If during this period symptoms become evident (fever or cough or there is high clinical suspicion according to the attending physician), they will perform a respiratory smear to detect the virus by PCR, according to the protocol established in each hospital for the detection, diagnosis and management of suspected cases.
- •
Smear test is not indicated if the patient remains asymptomatic, unless the clinical suspicion is very high. PCR is not recommended in asymptomatic contacts because it is not sensitive for the diagnosis of a latent infection. Therefore, if the result is negative, it really does not rule out that he may become positive and the worse consequence would be an early decision to withdraw isolation measures based on “false security”, putting at risk the rest of the patients and staff; if symptoms appear the test and isolation would have to be repeated. There is no test to rule out a latent infection, so the reasonable strategy would be to wait 14 days since the risk contact occurred, being under the basic isolation measures (gloves and masks for all patients), and do the test only if symptoms become apparent.
- •
The isolation measures of these patients are the same as if they had the diagnosed infection: contact and drops isolation, so they can be in the same room as the infected, always trying to respect 2m of distance between one patient and another., and all must wear gloves and a surgical mask.
- •
If the Center can offer isolation to close contacts patients, cases under study or confirmed cases that do not require hospital admission, the patients will be dialyzed at the center.
- •
In the event that the center does not have this possibility, these patients will be dialyzed in the reference hospital.
- 1.
Patients who do not require hospital admission will be dialyzed in the individual room designated for this purpose. Patients admitted to the hospital may undergo the hemodialysis session in the individual patient's room using portable hemodialysis monitor, as long as the room fulfill conditions of contact and drops isolation, with the staff using the recommended personal protective equipment (PPE) for COVID-19. If there is more than one patient with COVID-19, they can share the room.
- 2.
Hepatitis B isolation rooms used to dialyze patients with hepatitis B positive surface antigen should be used for patients suspected of confirmed COVID-19 only if the patient is positive surface antigen for hepatitis B.
- 3.
It is necessary to maintain a list of all health care personnel and patients who have been in contact with the patient. It is important to identify all healthcare personnel taking care of cases under study, probable or confirmed cases of coronavirus infection. The risk must be assessed individually by Occupational Health and the Epidemiological Surveillance Emergency Service. If the safety measures have not been followed, they will be considered close contacts and will be handled as such. To facilitate this task, it is convenient, as previously mentioned, that each nurse always have the same patients assigned in one shift.
- 4.
Reusable or non-critical disposable equipment should be used for patient care (e.g., blood pressure cuffs). If the equipment has been used on the patient, the equipment must be cleaned and disinfected before using it on another patient according to the manufacturer's instructions.
In general, the medical care of patients with respiratory infections without a diagnosis should follow standard precautions to prevent contact and eye protection against drops, unless the suspected diagnosis requires precautions for airborne infections.
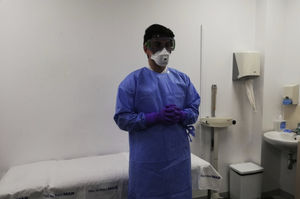
Evaluate equipment supplies available for individual protection, including masks FFP2 (Fig. 2). Eye protection can include a surgical mask with a protective screen.
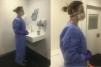
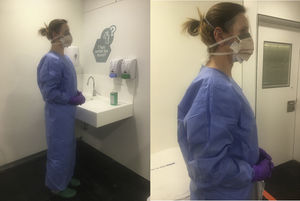
Personal protective equipment (PPE), consisting of a pair of powder-free long-sleeved nitrile gloves, a long waterproof gown, a FFP2 mask, and a full-screen surgical mask. This list of individual protective equipment is under permanent review depending on the evolution and new information available on SARS-CoV-2 disease.
This includes the use of:
- •
Waterproof gown covering 360 degrees, which should be worn over or instead of pajamas normally used by hemodialysis staff. This is particularly important when accessing a vascular access to connects and disconnects, helping the patient to get in and out of the room and cleaning the room. The same gown should not be used for the care of more than one patient, except if they are isolated together (cohort isolation).
- •
Gloves, long if possible, to cover and close the sleeves of the gown.
- •
Facial mask: mask FFP2 and surgical mask with screen.
- •
Only when preparing to generate aerosols (anebulization, mechanical ventilation, bronchoscopy, IOT, suction of secretions), it is required the use requires mask FFP3 (with exhalation valve) and integral glasses of full protection (Fig. 3). The personal glasses and contact lenses are not considered appropriate eye protection. Reusable eye protection (e.g., glasses) must be cleaned and disinfected before reuse according to the manufacturer's instructions. However, it is recommended to use disposable material with the PPE.
Fig. 3.If aerosols are to be produced (administration of nebulisations, mechanical ventilation, fiberoptic bronchoscopy, orotracheal intubation, aspiration of secretions, etc.), a FFP3 mask (with exhalation valve) and full protective glasses are required. It is recommended that all material be disposable. If long sleeves are not available, use the isolation gown (green) and add a plastic apron.
Environmental disinfection:
- •
Follow the protocol for decontamination, conservation and residues disposal (including clothing) commonly used for other types of microorganisms with risk of spread through contact and drops.
- -
The residues are considered Class III or Special Biosanitary waste (Group III, similar to tuberculosis).
- -
There will be 60-liter containers inside the box/room for the disposal for all patient residues, including the PPE used by healthcare professionals. Once it is full, the cleaning staff will be notified immediately for their removal and replacement.
- -
To avoid manipulation of urine and feces of the patient, it is necessary to use absorbent bags that will be placed on the wedge and/or in the urine bottle. Subsequently they will be closed and thrown into the group III waste container.
- -
Surfaces in contact with the patient or their secretions will be cleaned and disinfected (including the chair or stretcher, the waiting room and the elevator that has been used for the transfer; walls, keypads and elevator floor) according to the protocol of each hospital. Cleaning and disinfection will be performed with a disinfectant made of sodium hypochlorite solution containing 1000ppm of active chlorine. The viruses are inactivated after 5min of contact with normal disinfectants such as household bleach.
- -
Cleaning personnel must be adequately protected with PPE with a FFP2 mask.
- -
Devices and medication:
- •
Devices and materials used in the dialysis session should be used in a single patient and should be cleaned and disinfected on common clean area before being stored.
- •
The materials and medication found in a hemodialysis stations should only be used in the patient dialyzed in that station and should never be returned to the common clean area or used with other patients, without being previously disinfected.
- •
Ordinary carts should not be used to carry medication to patients.
- •
If trays are used to carry medication to individual patients, they must be cleaned between patients.
- •
Clean areas should be clearly separated from contaminated areas where contaminated material is being handled.
- •
Additional prevention measures carried out in China and Taiwan included not give food to patients during the session of hemodialysis.
Monitors and surfaces:
- •
External surfaces (chairs, beds, tables, monitors) should be cleaned and disinfected.
- •
The external surfaces of the monitors are the most likely source of contamination. Once the patients are connected and whenever a patient is being attended, the surface of the monitors will be cleaned with soap and water, and then a disinfectant with a sodium hypochlorite solution containing 1000ppm of active chlorine will be applied. These viruses are inactivated after 5min of contact with normal disinfectants such as household bleach.
- •
Especial attention should be paid in the cleaning and disinfection of control panels of dialysis monitors and other surfaces that are frequently touched and therefor are potential contaminants.
- •
It is essential the early identification of individuals at risk, preferably before being transported to the hemodialysis center. This is crucial for the prevention of transmission in the ambulance, waiting rooms and hemodialysis units.
- •
It is a priority to provide adequate training to patients and all personnel involved on the prevention and identification of COVID-19 in the different stages of hemodialysis (including transport from home).
- •
It is advisable to have systems that allow hemodialysis treatment to be performed in conditions of contact and drop isolation. There are different options (single room, portable ambulatory hemodialysis monitors).
- •
Health workers attending suspected cases or diagnosed with COVID-19 are responsible of maintaining a strict compliance with the standard precautions of contact and drop isolation and adequate personal protection (PPE).
The authors have no conflicts of interest to declare.
Please cite this article as: Arenas MD, Villar J, González C, Cao H, Collado S, Crespo M, et al. Manejo de la epidemia por coronavirus SARS-CoV-2 (COVID-19) en unidades de hemodiálisis. Nefrologia. 2020;40:258–264.