B-cell chronic lymphocytic leukemia (CLL-B) is the most commonly diagnosed leukemia in adults in Europe.1
Kidney involvement has been described at diagnosis with an incidence of 7.5%2,3 and 16.2% during the course of the disease.4 C3 glomerulonephritis (C3GN) is a rare disease characterized by accumulation of complement factors in the glomeruli due to overactivation and abnormal regulation of the alternative pathway of complement. One of the abnormalities commonly associated with this entity is the detection of a monoclonal gammopathy, being CLL one of the hematological diseases less commonly associated with C3GN.5
We present a case of a 68-year-old woman with overweight, hypertension and diabetes mellitus. She had non-proliferative diabetic retinopathy and hypertensive heart disease. Six months before she had the diagnosis of CLL-B with no clinical or laboratory criteria for targeted treatment.
She presented with uncontrolled hypertension, anasarca and respiratory acidemia due to type 2 respiratory insufficiency, progressing rapidly to respiratory failure and mechanical ventilation. Biochemical investigation showed worsening anemia and leukocyte count, acute renal injury, hyperkalemia, hyperuricemia and hypoalbuminemia. The urine sediment had leukocyturia, erythrocyturia and hyaline and granulous casts and 24-h urine protein was 5.6g. A renal ultrasound only showed discrete loss of cortical-medullary transition.
Pleural involvement by CLL was excluded. Serology studies for hepatitis B, C, VDRL and HIV 1 and 2 were negative. Immunologic studies showed decreased complement C3 levels with normal levels of C4. Anti-Neutrophilic Cytoplasmic Autoantibody (ANCA) were negative, cryoglobulins and anti-PLA2R (ELISA) were normal. Electroimmunosubtraction showed two bands with monoclonal characteristics (serum IgM/Lambda and IgG/Kappa and urinary IgG/Lambda type and free lambda light chains).
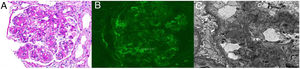
Renal biopsy with seventeen glomeruli, two of which were globally sclerosed and the rest showed a membranoproliferative pattern (Fig. 1A). Renal tubules had thickened tubular basement membranes, there was interstitial mononuclear infiltration without significant fibrosis and moderate arteriolar hyalinosis. Immunofluorescence study revealed mesangial granular deposits for C3 (++), C4 (+) and vestigial IgM (Fig. 1B). There was no Congo red staining nor green birefringence on polarized light. Electron microscopy revealed electron dense mesangial deposits (Fig. 1C). There was no evidence for deposits along the capillary walls and there was around 40% of foot process effacement.
(A) Glomerulus showing moderate mesangial widening and thickening of capillary walls, as well as double contours. (Periodic acid-Schiff stain (PAS) stain, 200×), (B) Immunofluorescence microscopy showing small granular deposits of complement (C3), mainly in the glomerula mesangium (×200). (C) Electron microscopy revealing electron dense deposits in the mesangial matrix (×8000).
A final diagnosis of C3GN was made and renal disease as an underlying immunological phenomenon related to CLL was assumed. A deletion of the TP53 gene was detected and she started treatment with Rituximab and high dose methylprednisolone. After 6 cycles she achieved a complete hematological remission (Table 1) along with stabilization of renal function and marked improvement in the proteinuria.
Biochemical variations along the disease curse.
| Hematologic and biochemical parameters | Leukocytes (×103/μL) | Lymphocytes (×103/μL) | Hg (g/dL) | Platelet (×103/μL) | sCR (<0.9mg/dL) | sU (10–50mg/mL) | Albumin (3.4–4.8g/dL) | 24-h protein (g/day) | Urine protein (mg/g crea) | DHL (U/L) | B2 M (mg/L) | C3 levels (mg/dL) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| At diagnosis of CLL | 18.6 | 10.4 | 11 | 174 | 1.3 | 97 | 3.1 | – | 7700 | 416 | 4.6 | – |
| At hospital admission | 63.9 | 40.9 | 7.5 | 131 | 1.8 | 90 | 2.9 | 5.6 | 9200 | 178 | – | 58 |
| After treatment | 7.6 | 1.6 | 11 | 140 | 1.2 | 74 | 3.8 | 0.1 | 3076 | 182 | – | 78.2 |
B2M: beta-2 microglobulin; DHL: lactate desidrogenase; Hg: hemoglobina; sCr: serum creatinine; sU: serum urea.
The first case of kidney disease in CLL was reported in 1957 by Scott et al. in a patient with nephrotic syndrome.6 After that, several glomerular diseases have been associated with CLL and depending on the type and stage of the disease, the spectrum of kidney pathology can be particularly wide.7 It can occur by diverse mechanisms such as parenchymal infiltration, extrarenal obstruction, tumor lysis syndrome, glomerulopathies, renovascular disease, electrolyte disorders and medication side effects.2
A chronological relationship with a suspected pathophysiological link and a parallel evolution of glomerulopathy and malignancy are suggested of paraneoplastic glomerulopathies.8,9 Their pathophysiology is thought to be multifactorial10 since monoclonal protein secreted by B-cell clone can either be directly involved in the pathogenesis of the lesions, as is seen in fibrillary glomerulopathy, immunotactoid/microtubular glomerulonephritis, AL amyloidosis and type I/II cryoglobulinemia, or indirectly, as in cases of membranoproliferative glomerulonephritis (MPGN) not related to cryoglobulinemia.4,11
MPGN is by far the most common glomerular lesion described, followed by membranous nephropathy, minimal change disease and amyloidosis. Cases of MPGN presenting as C3GN, as the case here discussed, have also been reported.12 One of the abnormalities commonly associated with C3GN is the detection of a monoclonal immunoglobulins. In this case, impaired regulation of the alternative pathway of complement is caused by monoclonal immunoglobulins and the MPGN pattern on kidney biopsy is the most frequent.13
The presence of kidney disease can interfere with treatment strategies and outcomes. Therapy is only required for patients with active or symptomatic disease, or with advanced Binet or Rai stages.14
Renal prognosis of C3GN remains poor, since 40% of patients progress to end stage renal disease 8–10 years after diagnosis and treatment is not well stablished.15
In conclusion, kidney involvement in patients with CLL could be more frequent than previously thought. Since it may present with a variety of pathology patterns and only a few of them predictable on clinical basis, kidney biopsy is essential. C3GN is rarely seen and renal prognosis as well as response to therapy is unknown. The report of these cases is of major role for better understanding the pathophysiology of this disease and in order to improve treatment and prognosis offered to this rare group of patients.