Arterial hypertension is prevalent in the black population in the United States. It is directly related to cardiovascular and kidney damage. Its pathogenesis is complex and includes the high incidence of obesity, salt sensitivity and the activation of the renin-angiotensinaldosterone system. This complexity requires a therapeutic combination that includes changes in dietary habits and appropriate antihypertensive regimes. The International Society of Hypertension in Blacks recommends initiating dietary intervention for values of systolic/ diastolic arterial blood pressure above 115/75mmHg and maintaining arterial blood pressure below 135/85mmHg using appropiate antihypertensive medication. The most adequate antihypertensive drug for this population has yet to be determined.
La hipertensión arterial es prevalente en la población de raza negra en los EEUU. Presenta una relación directa con el daño cardiovascular y renal. Su patogenia es compleja e incluye la alta incidencia de obesidad, sensibilidad a la sal, y la consecuente activación del sistema de la renina, angiotensina y aldosterona. Eso hace que requiera una combinación terapéutica que incluye cambios dietéticos y regímenes antihipertensivos adecuados. La Sociedad internacional de la hipertensión en pacientes de raza negra recomienda iniciar dietas de control para valores de tensión arterial sistólica/diastólica por encima de los 115/75mmHg y mantener una tensión arterial por debajo de 135/85mmHg con el uso de medicación antihipertensiva idónea. El fármaco antihipertensivo adecuado está por determinar en esta población.
The prevalence of hypertension (HTN), particularly difficult to control blood pressure (BP) and earlier onset of hypertension, is significantly more common in African Americans (AA) than whites. Sub-clinical manifestations of pressure-related target organ injury are also more common in AA than whites, even at blood pressure levels well below conventional HTN thresholds. This translates in the disproportionate occur rence of adverse subclinical and clinical pressure-related complications in African Americans that are consequence of suboptimal levels of blood pressure control in those with established HTN coupled with longer duration of blood pressure over their life span. According to the most recent National Health and Nutrition Examination Survey (NHANES) data, the proportion of treated patients with controlled HTN among blacks were similar to those for Hispanics but significantly lower than whites.1 These racial differences in control rates cannot be attributed to differences of awareness and treatment (reportedly been higher among blacks), nor the use of nonpharmacological/behavioral management, availability of health-insurance, economic barriers, or access to healthcare.2 The pathogenesis involves multiple mechanisms with the interaction of different factors like obesity, salt sensitivity, renin angiotensin system, and endothelium vascular response among others. The International Society on Hypertension in Blacks recommends a blood pressure goal of <130/80mmHg. The majority of AA hypertensive patients will require combination antihypertensive drug therapy to meet BP goals. Monotherapy with a thiazide diuretic or a calcium channel antagonist has consistently lowered BP in this population. Angiotensin converting inhibitors and angiotensin two blockers could be used in combination with diuretics for optimal BP control and renoprotection in patients with chronic diabetic and non-diabetic kidney disease. The final goal encompasses the optimal drug combination for the control of BP and protection of target-organs. With the influx in Spain of immigrants from the African continent and Caribbean countries of African ancestry, the present review will try to explore the epidemiology, pathogenesis and treatment options in our African American (AA) population that will helps us better understand and elaborate the best therapeutic options for our patients.
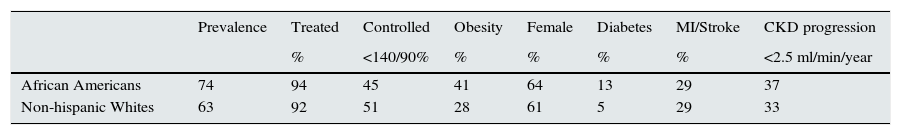
EpidemiologyHypertension in AA is a major clinical and public-health problem because of the high prevalence and premature onset of elevated blood pressure in this population. Moreover, the common occurrence of pressure related target organ injury and high prevalence of comorbidities such as diabetes mellitus and chronic kidney disease, markedly increases the likelihood of morbidity and mortality in this group at any given blood pressure level (Table 1).
Studies have shown causality between HTN, increased Body Mass index (BMI), and Sodium intake in the general population. Hypertension in the United States (US) black population has been associated with obesity (especially in women). Excess dietary sodium intake coupled with salt sensitivity, lower dietary potassium intake, excess alcohol intake, and an inadequate intake of dietary fruits and vegetables correlate with this assertion.3
Changes in vascular anatomy can have a deleterious effect in blood pressure control and increase the incidence of cardiovascular events. Risk factors such as arterial stiffening and increased peripheral resistance may contribute to the development of HTN and cardiovascular disease in the general population and particularly in AA.4 Cross sectional studies, demonstrate that healthy black men can present with an increased degree of carotid hypertrophy, stiffness of the central arteries, heightened resistance artery constriction/ blunted resistance artery dilation, and greater arterial wave reflection than their white counterparts.5
Ethnicity has played a role in the prevalence of HTN in certain geographical areas. Data, demonstrating lower prevalence of HTN among populations of African descent from the Caribbean and rural continental Africa relative to those in the US, supports the hypotheses that environmental factors represent an important role in the development of HTN in blacks living in the US.6 This geographic variation in HTN prevalence could be attributed to differences in body mass index (BMI) and dietary sodium: potassium ratio. For example higher incidence of HTN have been seen in blacks born in southern versus northern states.
In addition to environmental factors, genetic factors can contribute to HTN development and progression in blacks. Genetic underpinnings that may increase the tendency to retain sodium include: Epithelial sodium channel polymorphisms leading to cellular sodium transport defects, lower levels of renin and kinins and lower levels of natriuretic vasodilator prostaglandins amongst others.3 Multiple single nucleotide polymorphisms that may be significant in their relationship to systolic blood pressure have been also identified (SLC24A4 and CACANA1H) and are reasonable potential candidates for BP regulation involving sodium, potassium, and calcium exchanges.7
Blacks in the US demonstrate excess cardiovascular morbidity and mortality relative to whites.8 In the recent coronar y arter y r isk development in young adults study (CARDIA),9 a long-term multicenter US study that enrolled young adults (ages 18-30), the cumulative incidence of systolic heart failure during 20 years of follow-up was greater among blacks (1.1% in black women and 0.9% in black men) that among whites (0.08% in white women and 0% in white men; P=0.001 for blacks versus whites) and was directly related to the increased burden of HTN. Specifically, 75% of blacks who developed systolic heart failure had HTN during the first 10 years of the study versus only 12% of blacks without HTN (P<0.001). Further, elevated BP remained a significant risk factor for systolic heart failure throughout the study (P<0.001). In the Jackson cohort of the Atherosclerotic Risk in Communities (ARIC) study, which included 1729 middle-age black subjects, echocardiography revealed a prevalence of left ventricular hypertrophy (LVH) of 37% in black man and 41% in black women.10 Racial causality was not feasible since there were no whites in the cohort. Other population-based studies have shown increased prevalence of LVH in blacks versus whites. Prevalence that persists even after adjustment for conventional demographics and clinical risk factors, including age, gender, height, and BMI.11 Left ventricular mass and its geometry are independent and strong risk factors for cardiovascular morbidity and death. The cohort study by Liao et al. evaluated 1089 black patients, who underwent both coronary angiography and M-mode echocardiography, and found that LVH without coexistent obstructive coronary artery disease was associated with lower survival rate than patients with single-vessel disease and similar survival rate as multiple vessel disease.12 Baseline data from the Multi-Ethnic Study of Atherosclerosis (MESA), which enrolled 6814 patients from four racial/ethnic subgroups (whites, blacks, Hispanics, and Asians) with no cardiovascular disease, revealed direct relationship between the ventricular mass and well establish risk factors such as systolic blood pressure, current smoking, exercise, BMI, and diabetes.13
As described above. The cardiovascular and renal consequences of HTN are greater in blacks, relative to their white counterparts. Structural vascular abnormalities as well as genetic, geographic, and environmental factors may play an important role. The relationship between LVH and cardiovascular outcomes is particularly strong. These findings underscores the urgent need to successfully treat hypertension in the black population with agents that could reverse LVH.
PathogenesisThere are several pathophysiological mechanisms linked to the development of HTN and are disproportionately prevalent in selected racial/ethnic groups like AA (Table 2).
Obesity contributes significantly to HTN in all populations. Is more prevalent in both AA and Hispanics, particularly in women, compared with whites.14 One in six AA women are considered extremely obese (BMI>40kg/m2). This prevalence is almost fourfold higher than that of their white or Hispanic counterparts. Obesity related physiological effects that contribute to this BP phenotype include; enhanced sympathetic activity, altered salt sensitivity, and resistance to antihypertensive drug therapy, not to mention chronic renal injury due to glomerular hyperfiltration.15
Salt sensitivity is prevalent in AA, particularly those with HTN. Conceptually defined as a rise in BP during salt administration and/or a fall in BP when it is restricted. Weight loss ameliorates salt sensitivity at least among overweight Caucasian adolescents.16 Salt sensitivity has also been linked to a lesser fall in nocturnal BP (no-dipping) as well as to microalbuminuria and other pressure-related target-organ injuries in AA.
The role of the renin-angiotensin system (RAAS) in AA has not been clearly defined but the pattern of excessive RAAS dependent target-organ injury (LVH, CKD/proteinuria) in AA, showcases the importance of the RAAS in this population. This does not explain the lack of BP reduction with the use of ACE inhibitors compared with diuretics.17 A possible reason is that low renin levels increase the vascular production of angiotensin II promoting the fibrotic effects of aldosterone. Normotensive AA patients present with activation of the RAAS with higher aldosterone levels in comparison with whites. and AA with non-diabetic nephropathy experience less renal events when treated with an ACE inhibitor.18 Angiotensin two blockers in combination with a thiazide diuretic are as effective as calcium channel blockers (CCB) and thiazides in reducing BP in obese hypertensive AA.19 A combination of a CCB and a RAAS blockade in uncontrolled BP(>15/10mmHg of baseline 130/80) is indicated in AA hypertensives, in the absence of compelling indications for another drug class. Paradoxically the hypothesis behind vitamin D deficiency and incidence of HTN has been linked to activation of the RAAS in this population and its supplementation could suppress its activity and maybe control blood pressure.20
The endothelium presents as a target to the deleterious effects of RAAS activation. Endothelium-dependent and independent vascular responses are abnormal in AA compared with whites.21 There are also explanatory data suggesting that the bioavailability of nitric oxide is lower in AA than whites even though AA have much higher endothelial-derived nitric oxide synthase (eNOS) activity.22
Resistant HTN is more prevalent in AA than in Whites.23 They manifest the characteristics comorbidities (albuminuria, depressed kidney function, obesity,target-organ injury, diabetes, and severe BP elevations) that have been linked to antihypertensive drug resistance and therefore lesser HTN control.23 Wether poor BP control reflects true resistance HTN or other contributory factors such us lack of compliance or low socioeconomic status remains to be determine.
Obesity, salt sensitivity, RAAS, and endothelial activation represent different factors affecting the pathogenesis of HTN. The understanding of how this factors influence BP will guide the development of treatment protocols that will optimize the way we implement diet, physical activity and drug therapy. Elucidating this complex pathogenesis will also help guide therapies in the future.
TreatmentOptimal treatment of HTN requires an approach that encompasses multifactorial lifestyle modifications (weight loss, salt,alcohol restriction, and increased physical activity) plus drug therapy. The consensus statement on the treatment of HTN in AA from the International Society on Hypertension in Blacks (ISHIB) recommends comprehensive lifestyle modification in all AA with a BP>115/75mmHg.23 This is the BP level above which epidemiological cardiovascular disease risk begins its upward inflection. In contrast to the JNC 8 recommendations for the treatment of HTN,24 the ISHIB target BP goals remain lower (<130/80mmHg), especially in certain risk groups (CKD,Diabetes,cardiovascular disease).25 The American Diabetes Association (ADA) recommends a target BP for diabetics of <140/90mmHg.26 Data that correlates from previous studies that showed fewer strokes in cohorts with SBP control below 10mmHg lower than baseline and <120mmHg respectively.27
There is also convincing data of renal outcomes for attaining mean arterial pressure (MAP) <92mmHg compared to MAP of 102-107 amongst AA with HTN and non-diabetic nephropathy (urine protein/creatinine ratio >0.22).18
We now present the different therapeutic options by order of importance and clinical efficacy. The focus of drug therapy in AA is centered on the BP lowering efficacy of single drug classes. Unfortunately the majority will not be controlled with a single agent. Monotherapy with a thiazide diuretic or a calcium channel antagonist has consistently lowered BP more effectively than b-blockers, ACE inhibitors, and angiotensin II type 1 receptor antagonists.28 As mentioned above, the majority of AA hypertensive will require combination antihypertensive drug therapy to control their BP and there are no discernable racial/ethnic differences in BP response to two-drug antihypertensive therapy if at least one of the drugs is either a diuretic or a calcium channel antagonist. Highly effective drug combinations contain either a diuretic or a calcium channel antagonist in conjunction with a RAS antagonist. In the ACCOMPLISH29 (avoiding cardiovascular events through combination therapy in patients living with systolic hypertension) study amlodipine plus benazepril showed superiority over hydrochlorothiazide (HCTZ) plus benazepril combination in the black cohort (n=1416) particularly in patients with cardiovascular risk factors and diabetes mellitus. Thus, there are a number of relatively ineffective antihypertensive drug combinations that should not be used as first line agents to control hypertension (ACE inhibitors or ARB alone, peripheral and central-acting adrenergic inhibitors) in this population, except if target organ damage is present (CKD, Diabetic nephropathy). It is important to understand that the attainment of a clinical benefit is somewhat dependent on patient adherence. This has prompted recommendations for the use of single-pill fixed dose combinations.
Diuretics play a prominent role in AA with refractory HTN. The reason for this is not plasma volume expansion despite the prevalence of a salt sensitivity state, since the effect is transient in animal and human models of HTN.30 The use of more than one diuretic will be needed to control BP particularly in patients with estimated glomerular filtration rate <40ml/ Min (eGFR). Hydroclorothiazide plus an aldosterone antagonist or amiloride are used in patients with eGFR>50mL/min/1.73 m2 and have shown benefits when combine with loop diuretics, particularly in patients with advanced heart failure. In patients with eGFR of 30-45mL/min/1.73 m2, the combination of a thiazide and a loop diuretic represents and effective option.31
In the recent revision of the ISHIB consensus statement on the management of hypertension in AA25,32 the use of chlorthalidone over HCTZ was favored due to the fact that it lowered BP more effectively than HCTZ on a mg per mg basis, especially at night (longer half-life). The downside being the pill burden, intravascular volume depletion and consequent pre-renal azotemia.
Given the high level of pre-treatment salt sensitivity and the salt retaining effect of many antihypertensives (particularly vasodilators:minoxidil), coupled with the prevalence of obesity in this population, comprehensive lifestyle modification that entails dietary salt, higher intake of potassium and weight loss should be implemented. The ladder could lessen salt sensitivity and restore the “dipping” nocturnal effect of BP.33
There are multiple side effects that need to be taken in consideration when using different antihypertensives agents. As previously stated before angiotensin converting enzyme inhibitors and angiotensin two blockers could be used in combination with diuretics for optimal BP control and renoprotection in patients with diabetic and non-diabetic kidney disease. The clinician should be aware that angioedema occurs more in AA than whites during ACE inhibition treatment. Angioedema is less frequent with the use of ARB or direct renin inhibitors agents.34
Hypertension treatment in AA has evolved during the years. The goal is to use the most effective drug combination for the control of BP and protection of target-organs. In order to comply with the ISHIB recommendations for reduction of BP, optimal management of HTN in AA will require the use of comprehensive life style modifications and individualized drug combinations.
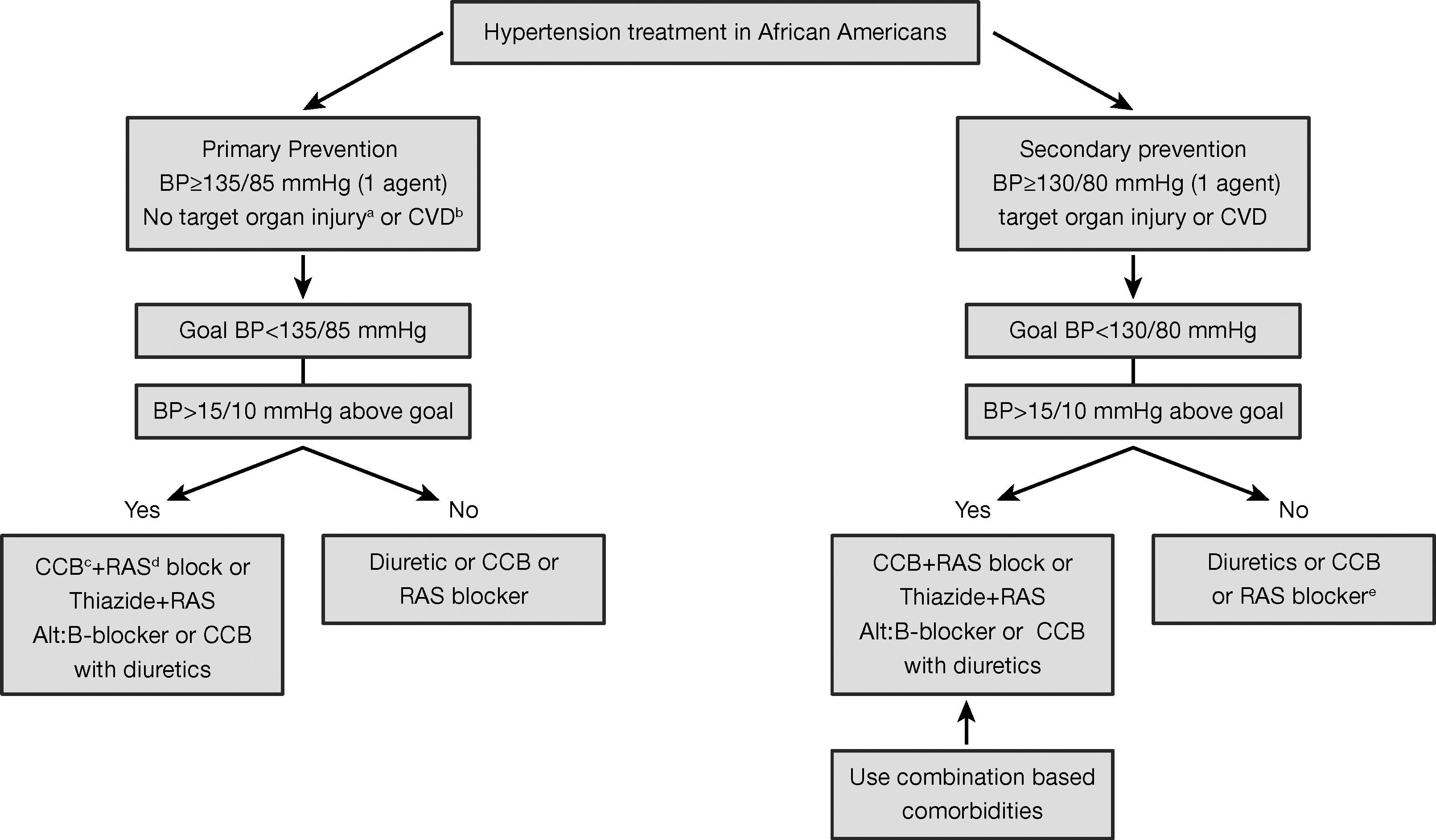
ConclusionThe prevalence of HTN is higher in blacks than in other race/ ethnic groups, with environmental and genetic risk factors playing an important role.35 The cardiovascular and renal complications of HTN are also greater in blacks relative to their white counterparts. Target organ damage such as LVH and renal failure are more common in blacks than whites, even after comparable levels of BP.31 The pathogenesis is multifactorial in nature, complicating therapeutic options and requiring a multidisciplinary approach. Emphasis should be placed on utilizing the most effective drug combination for the control of BP and protection of target-organs in this high risk population. The ISHIB consensus statement (Fig. 1) recommends a reduction in the BP target, even for the lowest risk AA population (<135/85mmHg) for primary prevention and <130/80mmHg for secondary prevention with target-organ damage present. As previously stated, this will require the use of comprehensive life-style modifications coupled with drug therapies tailored to different comorbidities.36
Treatment of hypertension in African Americans vs Whites. a Albumin:creatinine >200mg/g, eGFR <60mL/min 1.73 m2, left ventricular hypertrophy by electro-echocardiogram. b Heart Failure, CAD, peripheral arterial disease, stroke, TIA,abdominal aortic aneurysm. c Calcium channel antagonist. d Renin angiotensin or AT1 receptor blocker. e Agents are used with compelling indications.
- •
Hypertension is prevalent in the African American population.
- •
Epidemiology is influenced by ethnicity and genetics.
- •
Multifactorial pathogenesis influenced by obesity, salt sensitivity, activation of the RAAS, among other causes.
- •
Therapeutic antihypertensive options similar to whites with slight variations in blood pressure goals based on recommendations from the International Societ y of Hypertension in Blacks.
None.
Conflict of interestsThe authors declare that they have no conflicto of interests.